Bridging the Gap Between the Classroom and Practice Experiences
Clear exceptions and regular feedback are essential
by Taylor Chester, PharmD, PGY-1 Community-Based Pharmacy Resident, The University of Mississippi School of Pharmacy
For me, Advanced Pharmacy Practice Experiences (APPEs) were a major transition in pharmacy school, marking the shift from classroom learning to hands-on practice. For many health professions students, this is when everything begins to feel real. As a student, you are given the chance to apply what you’ve learned, build practical skills, and better understand your role in patient care before you graduate.1 Students spend years listening to lectures, taking exams, and engaging in structured learning before transitioning into authentic practice settings where they are expected to apply knowledge, communicate with other health professionals, and contribute to patient care. While this transition is exciting, it can feel overwhelming when expectations are no longer clearly defined.
When my fourth year of pharmacy school came, I was eager to learn and motivated to start my APPEs. I could finally apply what I was learning in the classroom to practice. As excited as I was to start, I also felt unsure of what would be expected of me from one rotation to the next. Universities often encourage students to email their preceptors about two weeks before the APPE to express their interest and what they hope to gain out of the experience. While this provides a helpful starting point, I learned that expectations communicated in-person are just as important. Uncertainty made it challenging, but also pushed me to become a more adaptable learner.
In college, our grades reflect foundational knowledge, but they don’t always reflect confidence, communication skills, or comfort working with patients, which are important goals of pharmacy education before students enter their APPEs. According to the Center for the Advancement of Pharmacy Education (CAPE) 2013 Educational Outcomes, pharmacy graduates are expected to demonstrate competencies such as communication, professionalism, problem-solving, and self-awareness.2
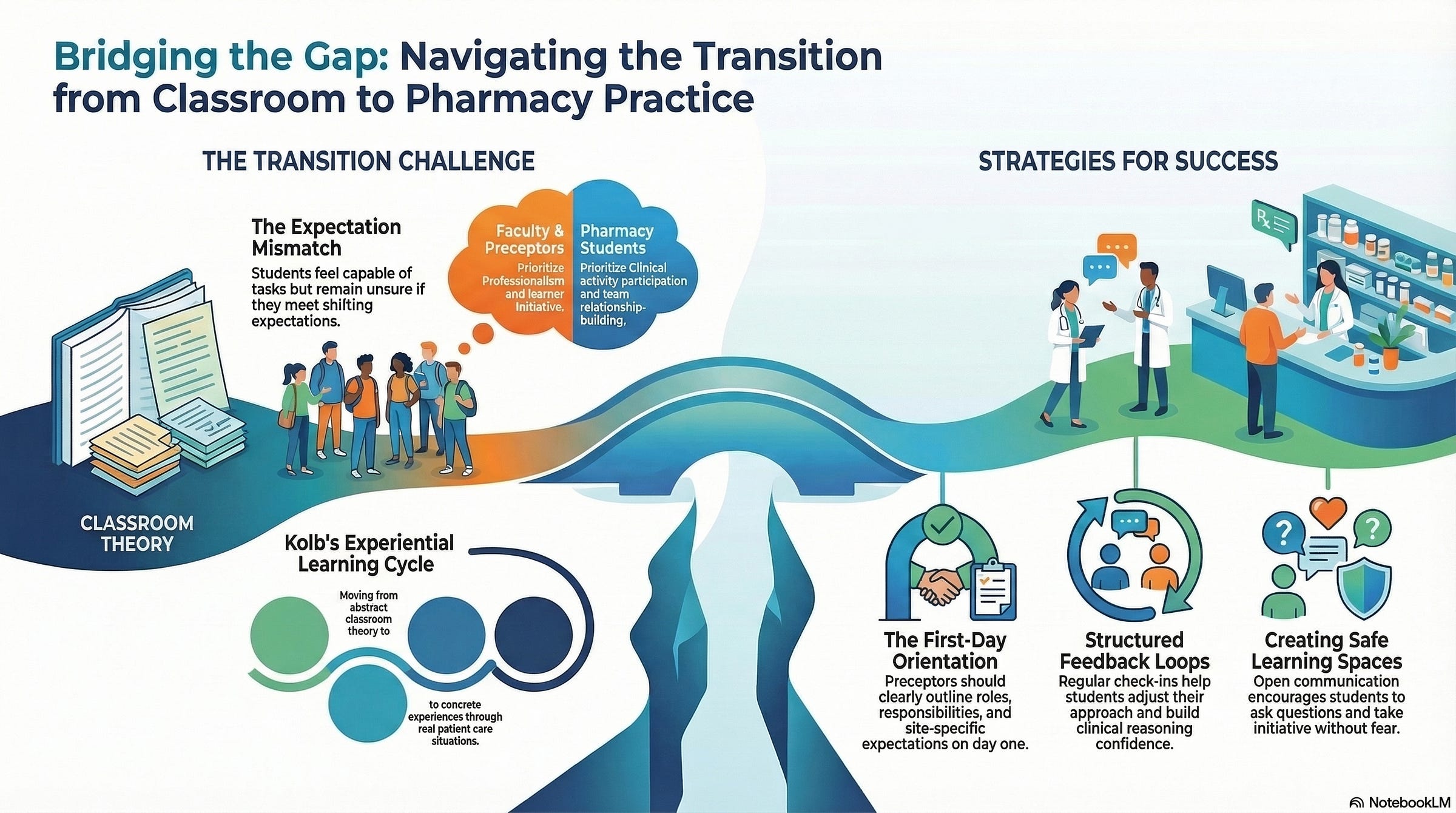
This transition from classroom learning to experiential learning can also be explained through Kolb’s Experiential Learning Cycle, which describes learning as a process involving four stages: concrete experience, reflective observation, abstract conceptualization, and active experimentation.3 During APPEs, pharmacy students move beyond abstract knowledge gained in the classroom and enter the stage of concrete experience, where learning occurs through real patient care situations. Reflecting on those experiences and adjusting approaches over time, during one APPE to the next, allows students to continue developing their clinical reasoning and professional confidence. These skills are difficult to fully develop through classroom instruction alone and are strengthened through experiential learning.
The disconnect between the classroom and clinical settings is analyzed in a qualitative study conducted by an interdisciplinary research team from the University of California San Francisco’s Schools of Pharmacy and Medicine.4 Using focus groups and individual interviews, the authors gathered perspectives from pharmacy students, preceptors, and faculty about preparedness for APPEs. To analyze participants’ responses, the researchers transcribed interviews and grouped recurring ideas and concerns. The study identified four key themes that influence APPE readiness: learner characteristics, participation in workplace activities, relationship-building within the healthcare environment, and workplace practices that help orient and support students.
After gathering the results, the researchers found that different groups emphasized different aspects of readiness.4 Faculty and preceptors tended to focus more on learner characteristics such as professionalism and initiative, while students focused more on participation in clinical activities and building relationships within the healthcare team. Some common themes found in the article included students describing uncertainty about what was expected of them early in the rotations, and preceptors acknowledging that expectations can vary widely across practice sites and be influenced by preceptors’ teaching styles.
The diversity of participants synthesized multiple viewpoints and helped explain why expectation mismatch was such a recurring theme. This mirrored my own experience during APPEs. Like many students in this study, I often felt capable of completing tasks but unsure whether I was meeting expectations, especially when those expectations shifted from one rotation to the next. At first, I thought this challenge was due to my own lack of effort or knowledge. This study helped me realize this challenge is common.
My APPE experiences pushed me to become more agile in my approach to learning. An example of this was presenting patient cases, which were structured very differently on my acute care rotation compared to my ambulatory care rotation. Of course, these were two different practice settings, but there were big differences in my preceptors’ expectations, such as the depth of patient information, the use of slide presentations versus Microsoft Word documents, and the disease-state focus.
Faculty and preceptors play a major role in shaping how students experience APPEs. One of the biggest differences I noticed across these experiences was how supported I felt based on how preceptors communicated and interacted with me as a learner. When preceptors took time to explain expectations, check in regularly, and encourage questions, I felt comfortable speaking up and taking initiative. Those rotations felt like safe spaces to learn rather than environments where I was afraid to make mistakes. On the other hand, when guidance was limited or feedback was inconsistent, it became harder to gauge whether I was meeting expectations, even when I was putting in effort. The preceptors who stood out most were those who treated APPEs as a learning experience and invested in mentorship, which helped me build confidence and begin to see myself more clearly in my role as a future pharmacist.
APPEs are one of the most important stages in pharmacy education because they mark the transition from understanding information to applying it in patient care. There are several practical strategies that educators and preceptors can use to support students during this transition.4 Preceptors should provide a brief orientation on the first day of the rotation, outlining expectations and responsibilities. Scheduling regular feedback sessions can also help students understand how they are progressing and what adjustments they should make before the end of the experience. Clear communication and regular feedback can make a significant difference in helping students feel supported while adapting to new practice environments.
Teaching approaches that connect classroom learning to real practice encourage students as they move into APPEs. When students are supported through confusing or unfamiliar situations rather than expected to navigate everything on their own, they are more likely to feel confident, adjust more easily, and grow into their role as future health professionals. Ultimately, APPE readiness is not about having all the answers on the first day, but about keeping an open mind, learning, adjusting, and growing with a supportive preceptor at your side.
References
1. Patterson BY. An advanced pharmacy practice experience in public health. Am J Pharm Educ. 2008;72(5):125.
2. Medina MS, Plaza CM, Stowe CD, et al. Center for the Advancement of Pharmacy Education 2013 educational outcomes. Am J Pharm Educ. 2013;77(8):162.
3. McLeod SA. Kolb’s learning styles and experiential learning cycle. Simply Psychology. Updated 2017. Accessed March 4, 2026.
4. Gruenberg K, Hsia S, O’Brien B, O’Sullivan P. Exploring multiple perspectives on pharmacy students’ readiness for advanced pharmacy practice experiences. Am J Pharm Educ. 2021;85(5):8358.