Integrating Research and Scholarship in Health-Professional Education Programs
The benefits are numerous
by Nicholas B. Yarbrough, PharmD PGY-1 Pharmacy Resident, G.V. (Sonny) Montgomery VA Medical Center
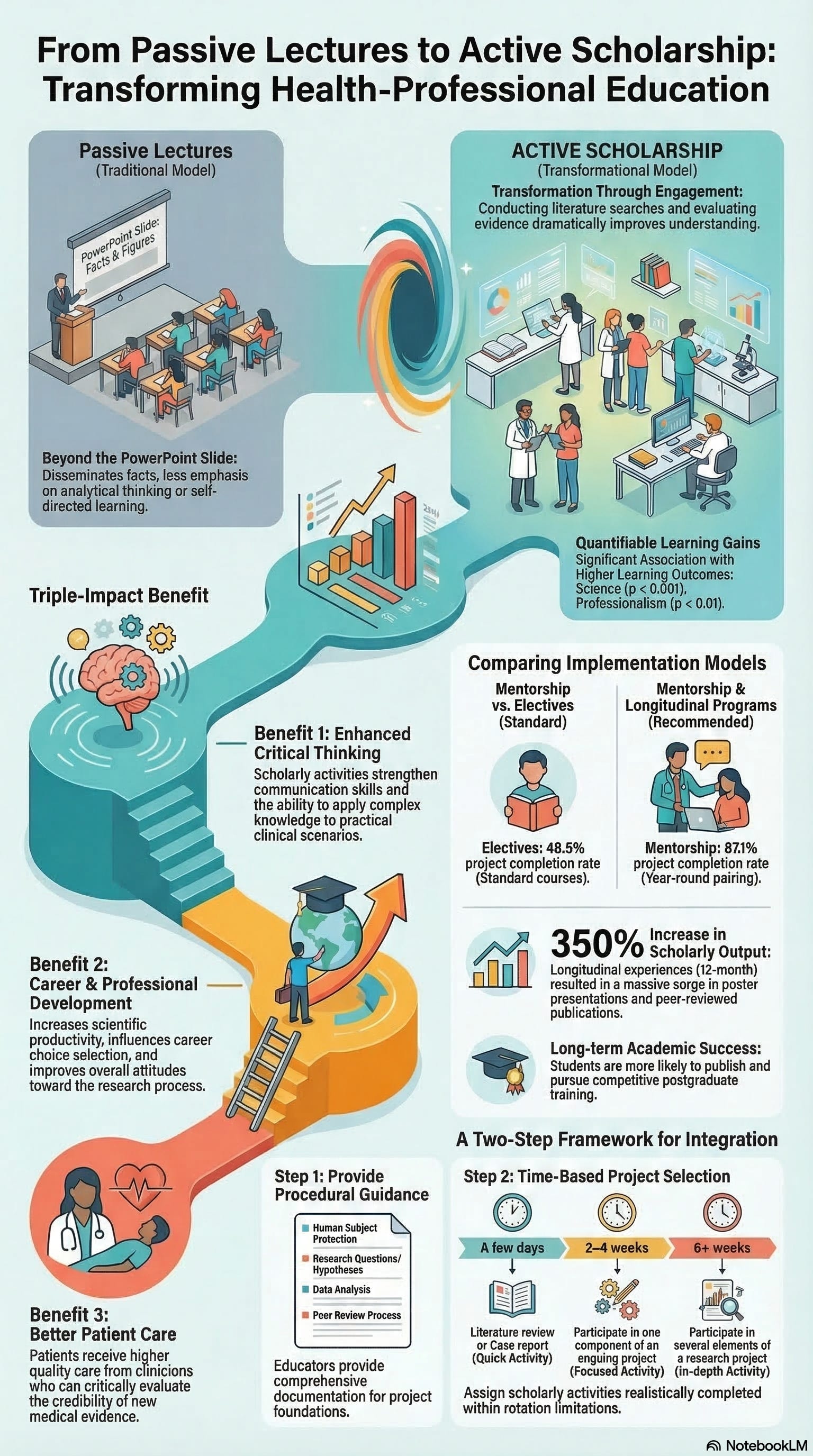
Everyone remembers the feeling of downloading PowerPoint slides full of information before an intense lecture – feeling overwhelmed, overstimulated, and over it. I was no different. I thought this was what learning was all about: one reads, hears, studies, and is then tested on the information. While this approach is time-honored and effective at disseminating facts, it often fails to foster a comprehensive, substantive understanding. Nor does it promote analytical thinking, self-directed learning, or problem-solving.
Research suggests that when students participate in scholarly activities, they gain skills that extend beyond the specific subject studied. These activities promote critical thinking, strengthen communication skills, and increase learners’ confidence in applying knowledge to real-world problems. For educators, incorporating scholarly engagement into training programs can be an effective strategy for promoting deeper and more meaningful learning.
My own perspective on learning changed during pharmacy school when I had the opportunity to collaborate with a faculty member on a scholarly project. I asked to work on a paper focused on a subject that I hated in the classroom. What transpired was transformational for me. Through the process of conducting literature searches, evaluating scientific evidence, and contributing to a scholarly writing project, my understanding of the subject improved dramatically. By the end of the project, I felt comfortable discussing the topic and applying the concepts in practice. This experience showed me something crucial: students learn best when they actively engage in research and other scholarly activities.
Empirical evidence supports this assessment. Zhang and colleagues sought to investigate the association between medical student research engagement and learning outcomes in their study, which included 10,062 medical students from 33 medical schools in China.1 They found engagement in research projects was positively associated with students’ learning outcomes, especially in the science and professionalism domains (p < 0.001 and <0.01, respectively).1 Amgad and colleagues drew a similar conclusion in their 2015 systematic review and meta-analysis, finding that medical student participation in research increased scientific productivity, influenced career choice selection, and improved attitudes toward research.2 The authors suggest initiatives aimed at increasing student involvement in research (e.g., a graduation thesis project or other forms of curriculum-required research) may produce positive results, though they stop short of endorsing any particular model.2
The literature varies on the best approach for implementing a research program into health-professional education (HPE). Kim and colleagues evaluated a program designed to increase student pharmacist participation in research by pairing students with research mentors throughout the academic year.3 In this program, students worked closely with faculty preceptors to design projects, collect and analyze data, and disseminate findings. The investigators compared outcomes from this mentorship model with a previously offered research elective. Students participating in the mentorship program demonstrated substantially higher research completion rates than those in the elective course (87.1% versus 48.5%).3 Additionally, students in the mentorship program were more likely to present their work, publish their findings, and pursue postgraduate training opportunities.3 Exploring a different approach, Michaelets and colleagues compared engagement in research before and after the implementation of a 12-month longitudinal research advanced pharmacy practice experience (APPE).4 They observed a 350 percent increase in poster presentations and peer-reviewed publications following implementation of the longitudinal APPE model (p < 0.01).4
Miller et al. provide a systematic approach to incorporating scholarly projects into clinical rotations or a dedicated research experience in two simple steps: providing students with a document that contains guidance on the research processes at the beginning of the experience, and selecting a scholarly activity based on the available time for the activity.5 In the first step, students should be given general instruction on research-related matters, including: human subject protection; literature searches; generation of research questions and hypotheses; consideration of how to test hypotheses; research proposals that include background, justification, methods, and analysis plan; the peer review process; data collection; data analysis; and dissemination of findings (e.g., presentation, poster, publications).5 Following this, students should also be assigned scholarly activities that can realistically be completed within the limitations of the time that is available during the learning experience.5 The authors offer loose guidance in this regard: those with only a few days to commit to research should complete a literature review or case report, those with 2-4 weeks should participate in one component of an ongoing project, and those with 6 or more weeks might be able to participate in several elements of a research project.5
By including scholarly projects in HPE, students have the opportunity to reap the empirically proven benefits for their knowledge, skills, and careers, including presentation skills, overall educational outcomes, and professional development. Some might argue, though, that the most important benefit is to future patients, who will have well-rounded clinicians who understand the research process, can evaluate the credibility of new evidence, and whom they can rely on for their health and well-being.
References:
1. Zhang G, Wu H, Xie A, Cheng H. The association between medical student research engagement with learning outcomes. Med Educ Online. 2022;27(1):2100039. doi: 10.1080/10872981.2022.2100039.
2. Amgad M, Man Kin Tsui M, Liptrott SJ, Shash E. Medical Student Research: An Integrated Systematic Review and Meta-Analysis. PLoS One. 2015;10(6):e0127470. doi:10.1371/journal.pone.0127470.
3. Kim J, McPherson SK, Koval P, et al. Evaluation of a fourth-year student pharmacist research process at a community teaching health system. Am J Pharm Educ. 2022;86(2):95-100. doi:10.5688/ajpe8440.
4. Michalets EL, Williams C, Park I. Ten‑year experience with student pharmacist research within a health system and education center. Curr Pharm Teach Learn. 2018 Mar;10(3):316‑324. doi:10.1016/j.cptl.2017.11.010.
5. Miller ST, Fulton J, Mastow M. Integrating structured learning and scholarly activities into clerkship rotations: A win-win for students and preceptors. Adv Wound Care 2014;3(5):400-403. doi: 10.1089/wound.2013.0504